
|
|
|
|
January 2013 Article of the Month
Blanchard, J. H., Dunlap, D. A. and Fitchett, G. "Screening for spiritual distress in the oncology inpatient: a quality improvement pilot project between nurses and chaplains." Journal of Nursing Management 20, no. 8 (December 2012): 1076-1084.
SUMMARY and COMMENT: This month's article attests to the value of chaplains conducting pilot projects for quality improvement as a way of moving into research, provides promising data on a method of engaging nurses around patients' risks for spiritual distress, and raises material for discussion about potential strategies for referrals to chaplains. The project was originally carried out by Judith H. Blanchard, Chaplain Clinical Leader at the Maine Medical Center in Portland, with Douglas A Dunlap (then a Chaplain Resident at the Maine Medical Center. though subsequently Chaplain at Franklin Memorial Hospital in Farmington, ME and Maine General Medical Center in Augusta). They are joined in authorship of the article by another chaplain, George Fitchett, Professor and Director of Research in the Department of Religion, Health, and Human Values at Rush University Medical Center, Chicago, IL. This work formed the basis of a workshop, "Screening for Spiritual Distress: A Quality Improvement Initiative," at the June 2012 annual conference of the Association for Professional Chaplains.
The project was spurred by the observation that the existing spiritual screening practice at the hospital -- a nursing assessment question, "Any spiritual practices that may affect your care?" -- rarely elicited a positive response from patients or referrals for spiritual care. A new two-question protocol was substituted, and 10 nurses were recruited on a 55-patient oncology unit to pilot it using the following algorithm [p. 1078]: 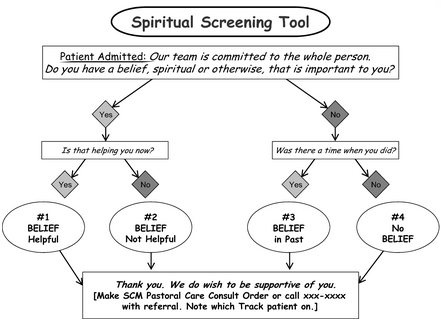 Each nurse was asked to screen all patients for whom they would conduct a nursing assessment in the 6-week period allotted to the screening, from late January to early March 2011. …Each nurse was provided with a script, [the] algorithm of the procedure…, and a pocket-sized, laminated card of the algorithm. They were instructed in how to put in an [electronic] consultation for spiritual care. …Weekly e-mails were sent to update participating nurses on the results to date, and to thank them for participating. In person check-ins were made as could be arranged, given that nursing schedules varied. [pp. 1079-1080]Referrals to the Spiritual Care Department included the screening code (1=belief helpful; 2=belief not helpful; 3= belief in past; and 4=no belief). The codes for "belief not helpful" and "belief in past" indicated an assessment of special risk for spiritual struggle/distress. Referrals were followed up promptly by chaplains who conducted their own assessment for spiritual distress. Among the results, 14 electronic referrals were made during the 6-week pilot. This stands in sharp contrast to the fact that a review of referrals "to the Spiritual Care Department over the 8 month period prior to this study (April–December 2010) indicated zero electronic requests by nurses in response to the nursing assessment spirituality item" [p. 1078, emphasis added]. In fact, while 8 of the 10 participating nurses had made referrals at some point in the past by phone, none reported being aware that electronic requests to Spiritual Care were available, much less how more efficient was the electronic process, which "generated a form printed out immediately in the Spiritual Care Office" [p. 1079]. Moreover, the 14 referrals represented a marked increase in Spiritual Care referrals from the involved oncology unit generally. Four of the 14 patients fell into the spiritual risk categories of Code 2 ("belief not helpful") and Code 3 ("belief in past,"), and they were all receptive to chaplains' visits. However, "those with Code 1 ['belief helpful'] also showed signs of spiritual need/struggle, and the distinction between Code 1 and 2 was not always clear cut" [p. 1080]. Spiritual needs evidenced in Code 1 patients included grief work around the loss of a spouse, fear before surgery, concerns about family members, depression, impending death and receiving Holy Communion. The one person with Code 3 – past belief – had a nursing referral, but the patient declined all chaplain visits, as did two of the three patients with Code 4 – no belief. The focus of this project was on nurse engagement and the piloting of a screening protocol. A continuation of this inquiry, a further project, should include a centralized gathering of and analysis of the spiritual assessment data for each screened patient. [p. 1080]The authors observe that the project may have affected the nurses' overall approach to referral for spiritual care, with that becoming more a function of "applying a set of screening criteria" [p. 1081] than merely passing along patients' requests. The new protocol may then have led the nurses to think of spiritual care referrals more in line with the way that referrals are generated for other services (e.g., respiratory therapy or social work), which do not depend upon "waiting for the unlikely event that a patient would request such services" [p. 1081]. Some of the nurses reported to us that the screening questions and the sequence provided them with terminology and a procedure by which they could make spiritual inquiry. They also reported that the project approach was an improvement over the existing procedure, because it led to more patient discussion than otherwise. [p. 1081]In addition, the project collected insightful comments from the participating nurses, and these may be interesting to chaplain readers. For instance, "The current [single-question] nursing assessment spiritual care item occurs near the end of a lengthy interview, and patients may be fatigued, desiring to end the interview as soon as possible," and "The yes/no format of these questions may inhibit a more substantial response" [pp. 1080-1081]. In light of the nature of the journal in which the article appears, the authors appropriately address "implications for nursing management," concluding: "The results of this project indicate that even busy nurses are responsive to explanations about the importance of screening for spiritual distress and training that helps them incorporate a brief spiritual screening protocol into their clinical practice" [p. 1082]. This is a small pilot, but it points toward improving the method for capturing patients' needs and making chaplaincy referrals, and it illustrates how an empirical quality improvement project may bring chaplains into closer collaboration with other disciplines. Suggestions for the Use of the Article for Discussion in CPE: The article begins nicely with a patient scenario and then covers background information that should be of interest especially to newer students. Even though the target audience is nurses, chaplains should be able to relate well. There is a reference to the Brief RCOPE, and one possible area of discussion might revolve around a practical consideration of how such a measure compares to the sort of screening protocol proposed by our authors. [For the Brief RCOPE, see the December 2012 and April 2009 Articles of the Month.] What is the difference between a measure and a screen in such cases? How might patients experience them differently? Is there anything about the particular screen that chaplains might want to incorporate into a pastoral visit? If a chaplain used the screening algorithm, would there be any tweaking of the wording? While the categories of "belief not helpful" and "belief in past" were given emphasis here as indicators of risk, chaplains in the project also found spiritual need/struggle present in patients who fell into the "belief helpful" category. What do students make of this? What might this say about the screening process in general? And, what do students think should happen for patients who would fall in to the "no belief" category? Finally, discussion might touch upon how a pilot quality improvement project like the one illustrated here may be a useful strategy for collaborative, interdisciplinary research. Related Items of Interest:
II. Though not stated in the article, a 2012 presentation by Judith Blanchard for the Maine Medical Center noted that the study addressed four aims for quality improvement in patient care that were set out by the Institute of Medicine in a 2001 report, Crossing the Quality Chasm: namely that care should be effective, patient-centered, timely, and efficient. Connecting one's work to larger, national research agendas is an excellent strategy for emphasizing the contribution made to the literature. Chaplains may wish to look at the Institute of Medicine report, which is available for download in book form from the National Academies Press.
III. This month article is part of a theme issue on spirituality in the Journal of Nursing Management [vol. 20, no. 8 (December 2012)]. Other articles in the issue include:
Spirituality: the Holy Grail of contemporary nursing practice," by Timmins, F. and McSherry, W. (pp. 951-957)
Spiritual care in nursing: an overview of published international research," by Cockell, N. and Mcsherry, W. (pp. 958-969)
An integrative review of spiritual assessment: implications for nursing management," by Draper, P. (pp. 970-980)
Who can give 'spiritual care'? The management of spiritually sensitive interactions between nurses and patients," by Kevern, P. (pp. 981-989)
Spirituality and spiritual care from a Careful Nursing perspective," by Meehan, T. C. (pp. 990-1001)
Creating conditions for good nursing by attending to the spiritual," by Biro, A. L. (pp. 1002-1011)
Perspectives of spiritual care for nurse managers," by Battey, B. W. (pp. 1012-1020)
A health services framework of spiritual care," by Daaleman, T. P. (pp. 1021-1028)
Discourses of spirituality and leadership in nursing: a mixed methods analysis," by Reimer-Kirkham, S., Pesut, B., Sawatzky, R., Cochrane M. and Redmond, A. (pp. 1029-1038)
The impact of workplace spirituality dimensions on organisational citizenship behaviour among nurses with the mediating effect of affective organisational commitment," by Kazemipour F. and Amin, S. M. (pp. 1039-1048)
How undergraduate nursing students learn to care for patients spiritually in clinical studies -- a review of literature," by Giske, T. (pp. 10491057)
Health-related religious rituals of the Greek Orthodox Church: their uptake and meanings," by Fouka, G., Plakas, S., Taket, A., Boudioni, M. and Dandoulakis, M. (pp. 1058-1068)
Spiritual leadership and spiritual care in neonatology," by Caldeira, S. and Hall, J.
(pp. 1069-1075)
|
If you have suggestions about the form and/or content of the site, e-mail Chaplain John Ehman (Network Convener) at john.ehman@uphs.upenn.edu
.
|